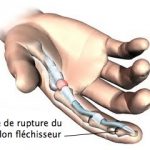
Whether the cause is domestic, an accident at work or a sporting activity, the functional and even aesthetic consequences of these injuries call for a preventive attitude at all levels.
In an emergency, the surgeon determines: the age of the injured person, any defects, dominant side, occupation, all data of importance in establishing the functional prognosis.
the accident: questioning provides information on the conditions in which the accident occurred: the time of the accident, which can be used to determine the operating time, and the causative agent:
- a clean, sometimes “reassuring” but often penetrating wound (glass, blade, metal edge);
- a jagged wound with possible associated contusion (router, circular saw, lawnmower…). Explosives, with damage often beyond any acceptable therapeutic resource, are a fearsome accident;
- a crushing wound (press, rollers, conveyor belt, wringer, etc.), which carries two aggravating risks: secondary skin necrosis and ischemic retraction of the hand’s intrinsic muscles;
- associated non-mechanical physical trauma (e.g. burns caused by a heating press);
- the position of the hand at the time of the accident, which determines the location of tendon sections in relation to the wound once the hand has returned to rest
The clinical examination may not be conclusive, but it does provide an initial assessment of the lesions:
- Fracture detection
- Search for tendon lesions
- Vascular and nerve damage
a simple radiological check-up in the emergency department is sometimes requested
Surgery is recommended as an emergency procedure, depending on the type of lesion to be treated at the same time. In some cases, lesions may require surgical treatment at a later 2nd stage of the procedure, far removed from the emergency episode and the inflammatory and healing phase of the 1st stage emergency operation (tendon graft, bone graft, skin graft, flap coverage, etc.).
The greater the number of damaged elements, the poorer the prognosis.
As a general rule, and in order of priority, we give priority to the vitality of the limb, then to function, and finally to aesthetics.
Amputation: The most frequent cases involve all or part of the distal phalanx. Depending on the affected finger or the terrain, they justify either the treatment that ensures the simplest closure (regularization, suture), or rather a plastic operation using an advancement flap to preserve the greatest possible length and pulpal function. The most serious cases are thumb amputations and multidigital amputations, which provide indications for microsurgical replantation whenever possible.
Some emergency measures to take in the event of complex trauma to the hand:
- Raise your hand above heart level.
- Compress the wound with a clean cloth, handkerchief, etc. for at least 15 minutes, without interruption (the time it takes for coagulation to occur).
- As a last resort (but in exceptional cases), apply a tourniquet just above the wound (between the wound and the heart).
- Use a fairly thick tie as a tourniquet (avoid cords). Use belts, ties, etc.
If the wound continues to bleed despite the tourniquet, the tourniquet is not tight enough.
Make a note of the time the tourniquet was applied. - Although it’s dangerous to keep a tourniquet tight for too long (more than 2 hours), we strongly advise against loosening it, even for a few seconds.
- In the event of amputation, remember that the amputated finger can be reimplanted (grafted) by the surgeon. So keep the amputated finger in a clean cloth, then wrap it in a watertight plastic bag.
Place the bag on the surface of a bowl containing water and ice cubes.
Never place the amputated finger in direct contact with the ice.
Contact the surgeon directly or go to the nearest health center.