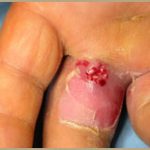
Panaris is an acute, primary cutaneous or subcutaneous infection of any constituent part of the finger.
Panaris occurs after inoculation following local trauma: a septic puncture (splinter), tearing of the periungual skin, and other dermatological affections.
The growth of germs leads to an inflammatory reaction (phlegmas stage).
Suppuration results from tissue lysis and the destruction of macrophages.
Staphylococcus aureus is the germ responsible for 2/3 of all cases of panicitis.
There are different clinical forms of panariasis:
- Subungual and periungual panarias account for 2/3 of all cases: this is the typical, easy-to-diagnose form, called “tourniole” when it circles the nail.
- Recurrent forms should suggest candidiasis or dermatophytosis.
- Pulpal panaris
- Dorsal panaris
- P2 lateral panaris

Evolution of a panariasis :
- Panaris Initial stage Resolution in 48 – 72 h
- Collected stage Healing in 2 – 3 weeks
- Recurrence = insufficient treatment
- Neglected panaris = spread to bone, joints or tendon sheaths
Treatment at the phlegmas stage :
At this stage, treatment is essentially medical: antiseptic baths 3 times a day, with or without antibiotic therapy. The patient is seen within 48 hours of treatment initiation for evaluation.
If signs persist or worsen, treatment will be surgical.
Treatment at the collection stage: wide excision of all necrotic tissue under anesthesia, combined with medical treatment and antibiotic therapy if there are associated general signs.
Early, appropriate treatment enables rapid, complete recovery within a few days. Poor treatment, delayed or neglected, can have serious functional and sometimes vital consequences.