Animal bites have become a veritable social phenomenon as the pet population continues to grow. Between 7% and 17% of patients consulting for an animal bite will develop a Pasteurella Multocida infection.
Cat bites account for 65% of infections.
POSSIBLE INJURIES
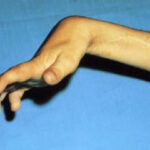
The initial appearance is not always alarming, and consultation of the injured is therefore often delayed.
Referring to the classification of Vilain and Michon, we distinguish between mutilating bites, decaying bites, and ponctiform or multi-punctiform bites.
It’s this last type that poses the most problems, because underneath its innocuous appearance, the actual seriousness of the injury may be underestimated by the bitten patient or by the doctor.
Their potential severity depends on :
- The aggressiveness of the biting animal and the extent of mechanical damage.
- The pathogenicity of the germs inoculated (107 to 109 bacteria/ml of saliva in mammals).
The constant presence of potentially pathogenic microbial flora in the oral cavity means that, by definition, a bite is infected.
There is no such thing as an aseptic bite. In mammals, the flora is mixed aerobic and anerobic. In humans, apart from alpha-hemolytic streptococci, anerobes are the most common: strepto, staphylo, Gram bacillus.
Pasteurelles or related P. Multicoda, M, EF4, 2J are found in the oral cavity in 70% of cats and 50% of dogs. The epidemiological calendar is typical, with hyperalgesic cellulitis appearing very early, between 1 h and 12 h after the bite, whereas pyogenic cellulitis is delayed until 48 h.
The diagnosis of inoculation pasteurellosis is therefore clinical, all the more so as bacteriological research is difficult in an emergency and its results delayed, and the self-sterilization of lesions is rapid.
POSSIBLE TREATMENT
Only systematic surgical exploration of all bites will enable careful trimming and, above all, a proper assessment of the lesions. Fangs can cut, sever or shred, and the wound must first be washed, then the soiled edges trimmed. The wound is then examined for tendon, artery or nerve lesions.
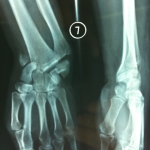
Fangs can penetrate the joint and contaminate it, damaging the cartilage, cutting into the external cortex and even fracturing, particularly in the digital segments.
The extent of skin involvement makes aseptic closure sometimes impossible. Closure should not be carried out under tension, or with economical trimming.
A flap may be necessary at a later stage. Although rarely observed, prevention of rabies and tetanus must be included in treatment. Initial antibiotic therapy is systematically applied postoperatively.
Human oral flora is sensitive to Penicillin G.
In cats and dogs, Pasteurelles are sensitive to Tetracycline and Penicillin A.
EVOLVING RISKS
Functional sequelae are dominated by joint stiffness, the causes of which are multiple and associated in dilapidating lesions, either through direct multi-tissue damage or algodystrophy, which is not surprising given the mechanical, bacteriological and psychological aggressiveness of the bite.
Non-specific delayed lesions :
Two clinical pictures of hand infection are quite evocative.
tenosynovitis and arthritis caused by common germs: the initial trauma has been forgotten or has gone unnoticed. It may be a simple skin erosion or a scrape that has since healed. A broad course of antibiotics has been taken indiscriminately.
Manifestations are non-specific; tenosynovitis can affect the extensors or flexors of the fingers.
Pain is often continuous, with progressive joint stiffening. There is edema with synovial thickening.
Functional impotence is variable. There are no general signs, and laboratory tests are mainly for elimination purposes.
MRI may show synovial thickening, but only cleaning and synovectomy will resolve the problem.
» Large, painful, inflammatory hyperalgesic hands » :
Moderately productive fistulas arising from osteomyelitic arthritis or phlegmon have been described in the literature. They occur after inadequate or insufficient initial treatment.
An even more misleading picture, at a distance from the initial trauma, is that of a stiffened hand with overall pain. The history of the disease may lead to a misdiagnosis, evoking an algo-neuro-dystrophic syndrome with noisy initial manifestations and evolution towards secondary stiffness, and X-rays showing osteoporosis due to non-use of the hand.
Several elements may suggest a pathology of inoculation by Pasteurrella Multocida:
- the search for an animal count, even if only slightly traumatic.
- the existence of a FIDR reaction to pasteurella antigen.
- positive serology with positive anti-pasteurella antibody levels. These examinations confirm the history of counting, but direct and current responsibility is not proven. The lesions are sterilized and the germ cannot be detected directly. Specific desensitization treatment may be proposed, but this is not harmless.
The best treatment is therefore an operation combining cleaning, trimming and exploration, coupled with a general course of antibiotics.