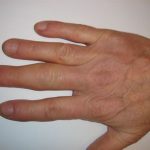
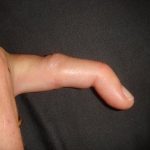
A severe sprain is a complete rupture of the ligament connecting the metacarpal to the first phalanx. The ligament detaches from the insertion of the first phalanx. If left untreated, the thumb is no longer stable, and the hand loses considerable strength.
Severe thumb sprains are most often caused by a violent deviation of the thumb, as in a skiing accident, but can also occur in a roller-skating fall, or simply in an ordinary accident.
Clinically: The thumb is painful, with minimal swelling. Examination by a physician looks for lateral instability of the thumb joint.

This sprain is very special in that the ligament loses all contact with its insertion due to an interposition.
X-rays look for a bone tear, which would indicate a complete ligament rupture that has carried away a small fragment of bone (from the first phalanx rather than the metacarpal). Most X-rays, however, appear normal.
Ultrasound can show bone stripping and joint effusion, as well as ligament displacement, in most cases, but can also produce false positives in cases of joint capsule rupture.
Some time after the trauma, a stress X-ray is performed to identify hyperlaxity, which indicates the need for surgery (> 30° or > 20° in relation to the opposite side).
MRI is the examination of choice for old ruptures and in doubtful cases.
In severe thumb sprains, surgery is essential to restore the ligament to its original position. Complete rupture of the medial ligament does not heal on its own. The ligament cannot be repositioned correctly, as it is impeded by the aponeurosis of the thumb adductor muscle, which interposes itself between the two ends of the ligament (Stener effect). After incision of the adductor aponeurosis, the broken ligament is sutured in place, or fixed through the first phalanx with an anchoring system. The repair must then be protected for 6 weeks to allow it to heal to the correct length.
When this procedure is performed within 3 weeks of the trauma, the results are good in terms of stability.
Operating protocol :
- Regional anesthesia,
- Outpatient hospitalization,
- Incision of the medial aspect of the joint and reinsertion of the ruptured ligament: reinsertion is always possible when the ligament is « fresh ».
- Post-operative immobilization of the thumb for three to six weeks.
- Rehabilitation sessions are usually required to restore full mobility to the thumb,
- No sport or effort with the thumb for 4 months.

Evolving risks
Failure to recognize the lesion:
This can occur for a variety of reasons, which we won’t go into here. The patient has difficulty using his thumb, to which he is often accustomed (sometimes it has existed for several years). Pain is rare. When using the thumb-index grip, the thumb “leaks” when the index finger is pressed.
Surgery may be proposed to stabilize the thumb:
Two possibilities:
- reconstruction of the ligament will be proposed if the joint is not damaged on X-ray: the results of this procedure are generally satisfactory.
- if the joint is altered on X-ray (signs of arthrosis): in this case, joint locking (arthrodesis) should be proposed. This blocking is definitive, and the function of the hand will be perfect despite the blocking.
Failure of initial treatment either :
- poor initial choice of treatment: immobilization of an injury that warranted surgical treatment,
- failure of ligament reinsertion,
Complications:
These can occur regardless of the type of treatment: thumb stiffness, algodystrophy, etc. They warrant specific treatment.